From cost center to value driver: AI-enabled nurse line services
(and where traditional models fall short)
Nurse line services were built to answer questions. The value-scaling opportunity for health plans lies in enabling members to navigate what comes next.
When a member calls a nurse advice line, they have a question: Is this serious? Should I go to the ER? What do I do right now? A good nurse answers those questions. But for most health plans, the interaction stops there – as does the value.
The member gets triaged, and they get an answer. Then they’re on their own to navigate a fragmented system, make care decisions without guidance, and often end up at the wrong site of care.
This is the gap at the center of traditional nurse line services. A failure of navigation, not triage.
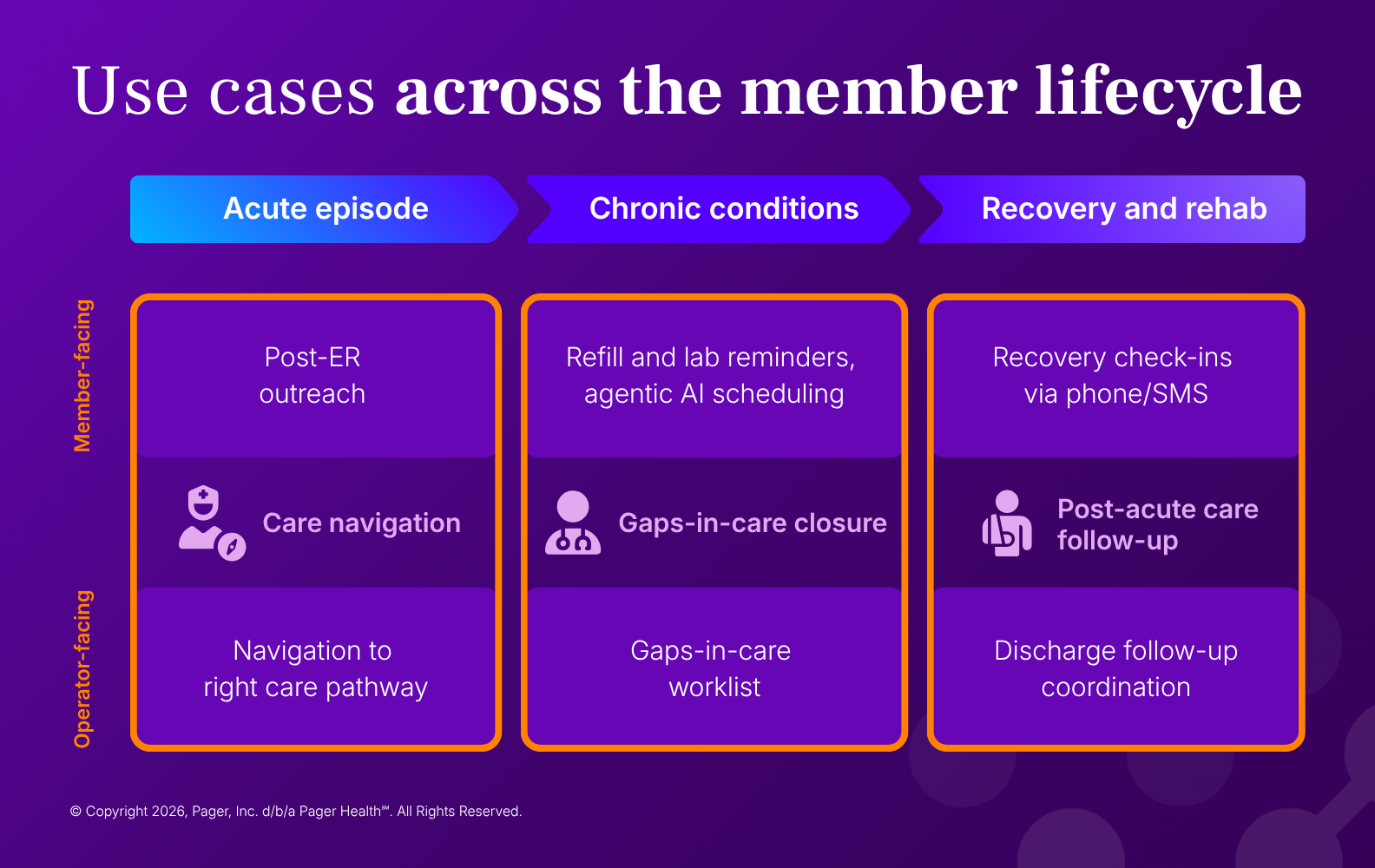
The opportunities in healthcare don’t only live in that first acute moment. They’re present across the full member journey, in whether:
A member with a chronic condition gets routed to the right specialist or defaults to the ER
Someone discharged after a high-risk episode gets the follow-up that prevents a readmission
A care gap gets closed before it compounds into something more serious and more expensive
Nurse line services that function as true care navigation deliver meaningfully stronger ROI than those optimizing the encounter alone.
Research has found that ED revisits drop from 10.3% to 7.6% when members receive a follow-up call within two days of discharge.¹ Another clinical study on discharge follow-up found readmission rates fall from 15.7% to 9.2% with post-discharge contact.² These are navigation outcomes, and in most traditional nurse line models, they go uncaptured.
The limitation of traditional nurse line services
The conventional model for nurse line services was designed for a different era. It’s reactive, phone-first, episodic, and often built around callback queues rather than proactive engagement.
In this model, a member wishing to speak with a nurse must call a generic phone number, wait for a callback, while the health plan hopes the information the member receives is actionable enough to guide them to the right site of care or next best action.
There’s no digital entry point for the growing majority of members who prefer to initiate care digitally, and no proactive outreach after a high-risk discharge. There’s also no engagement across the continuum of care except for the individual encounters that begin and end in isolation.
Optimizing call costs does not optimize the total cost of care.
Plans that focus exclusively on per-encounter cost metrics may run an efficient nurse line, but efficiency at the encounter level doesn’t prevent readmission or the gap in care that compounds into something more expensive.
Without encounter-level reporting on outcomes, there’s no way to credibly attribute savings or build a case for investment. That opacity is a feature of legacy models, but not a constraint health plans have to accept.
Pivoting to a care navigation platform
To ensure optimal clinical outcomes, nurses need the tools, intelligence, and infrastructure to do more, connecting what happens on a call to what happens next in a member’s care journey. This means digitally enabled, AI-supported, nurse-led navigation.
For health plans, this translates to cost savings, program value, and outcomes that can be measured and attributed.
Here’s what that looks like in practice:
Omnichannel access: Members connect how they want – phone, live nurse chat, or SMS. Direct, immediate access to a licensed registered nurse, not a callback queue.
AI-supported triage augments nurse-led navigation: Nurses are at the center of every clinical interaction and supported by AI to help them work through evidence-based protocols faster and with greater consistency, actively guiding members to the right site of care.
Closed-loop follow-up: Pager Health automates the follow-up workflow to reduce the burden on care teams. Predefined outreach protocols trigger post-discharge contacts and high-risk check-ins, with encounter-level reporting that captures what happened and ties it back to outcomes. This follow-up scales and generates data that proves ROI.
Lifecycle-wide engagement: Traditional nurse line services are reactive by design, built to handle a member’s condition in the moment. Clinical teams that broaden the aperture into proactive care navigation can drive meaningfully better outcomes. The same infrastructure that powers a triage call can support care navigation across the member lifecycle, turning a reactive safety net into a proactive clinical resource.
Proven outcome: $11.5M in program value for a health plan
When health plans build care navigation across the lifecycle into the nurse line experience, it scales up to something measurable, as a large health plan client discovered.
This U.S. plan, serving approximately 1.4 million members, relied on a reactive, phone-only nurse advice line with minimal navigation and sparse outcomes reporting. After partnering with Pager Health to develop a digital care navigation strategy, the plan implemented an AI-supported, nurse-led navigation model that delivered the following results:
$11.5M in program value across two years through site-of-care optimization with the model designed to scale as use cases expand across the lifecycle
68% of members reported they would have sought lower-value care without nurse guidance
86% reported symptom improvement following their nurse call or chat
The solution introduced omnichannel access, AI-supported triage, in-network navigation, and closed-loop digital follow-up, transforming the nurse advice line from a cost center into a measurable ROI driver.
Read the full case study to see how the health plan partnered with Pager Health to define and implement its clinical AI strategy.
Where real ROI emerges
Traditional nurse line services optimize the encounter. Pager Health optimizes the episode and the entire member lifecycle and transforms the nurse line from a reactive cost center into a proactive value driver.
AI-supported triage allows nurses to work faster and more consistently, while omnichannel access engages members rather than letting them drop off. Encounter-level reporting means plans can attribute the ROI which comes from comes from guidance, navigation, and follow-up working together.
As every use case runs on the same platform, health plans that start with a high-ROI nurse line entry point can expand into adjacent capabilities without rebuilding from scratch. The value compounds.
Explore Pager Health’s Clinical Navigator to see how your plan can reduce avoidable utilization, improve outcomes, and deliver measurable ROI.
Connect with Pager Health to explore how AI-powered orchestration can help your plan simplify member navigation, improve engagement, and deliver measurable ROI.